I have debated whether or not to make this post, because (1) the images are really graphic and (2) I’m reluctant to make my medical information public.
But if this can help educate people to the dangers of squamous cell carcinoma, and the hazards of relying on an HMO for medical treatment, then it will have been worth it. I’m putting the photos at the very end so as not to gross you out too much.
I noticed a “small pimple” on my left cheek in early December. By three weeks later, I was sure that it was no pimple. It was growing like gangbusters with a scaly surface. It looked like a little red crusty volcano. And at the rate it was growing, I wanted it gone yesterday.
I called my primary care physician on December 27 and asked for an immediate referral to a dermatologist. Protocol with my HMO is that I am supposed to see the primary care physician first, but I had no time to waste. Fortunately, my primary care doctor knows that I can recognize a squamous cell carcinoma, and she gave me an immediate referral. That was one week shaved off of the process of getting health care in today’s managed HMO system. I got the first available appointment with the HMO dermatologist, which was a bit over a week later.
In retrospect, I would have been better off bypassing my HMO and calling a dermatologist who did Mohs surgery. I would have had to pay out of pocket, but I would have gotten my cancer taken care of while it was still small instead of being given the run around from one doctor to another and another and another. As it is, I’m left with a scar on my face that is over two inches long. But I’m getting ahead of my story.
The HMO dermatologist did a shave biopsy, which doesn’t necessarily remove the cancer. By the time I saw her around January 6, my cancer was already 6mm by 11mm. I wish that she had cut a bit deeper and a little wider and taken it all, but my HMO won’t pay for removal without a biopsy confirming that it is cancer. Well, I knew it was cancer, and so did the dermatologist. She even subtyped it as keratoacanthoma type of squamous cell carcinoma, which is a very fast-growing and aggressive cancer. She said to return in a month.
The cancer looked gone after the biopsy. But the wound didn’t heal, a characteristic of cancer. I was forced to deal with twice daily wound care that consisted of washing the open wound with hydrogen peroxide, applying antibiotic ointment, and covering it with a bandage.
At the first sign that it was coming back–and that didn’t take long–I called the dermatologist and asked for an immediate referral to the Mohs physician. I wasn’t about to wait a month to see her and then wait even longer to get an appointment with the Mohs surgeon. The dermatologist had informed me at the time of the biopsy that my HMO doesn’t have any Mohs surgeons on staff and that I had to go outside the system for that type of surgery.The HMO pays for the surgery, of course, but it has to be with one of the Mohs surgeons that they contract with.
With the Mohs technique, the doctor does cryosections of the tumor and examines them under a microscope to make sure that all of the margins of the tumor are gone. She also looks at the base of the tumor, the part opposite the surface, to make sure that she got all of the “roots.” Tumors can send long “fingers” of cancerous tissue down deep into the normal tissue. If any cancer cells are left behind, then the cancer will return.
The HMO dermatologist gave me a referral to a Mohs surgeon dermatologist that my HMO contracts with for the surgery, but my HMO won’t pay that doctor to close the wound. I had to see a plastic surgeon within the HMO system for wound closure, which meant going to a different office in a different building later in the day, and getting yet another round of local anesthetic injections. Unbelievable.
My HMO decided that this wasn’t an emergency, and put me into the 5-day approval process. I straightened them out about that. I got immediate approval and shaved another week off of the time it took to get treatment.
Unfortunately, I had to see both of those doctors for consultations before they would schedule the tumor removal. That took a week. Scheduling the surgery took another week, and I was only able to get it scheduled that fast because of a cancellation. Meanwhile, the cancer cells were doubling every day and my biopsy site was not healing.
It was January 31 before I got the Mohs surgery, a month and a couple of days after my first phone call to my primary care physician. In the world of HMOs, that’s remarkably fast. Most people don’t get treatment until 2-3 MONTHS after the initial visit.
But by Jan. 31, my tumor was huge. The round incision to remove the tumor left a hole the size of a quarter in my face. Note that this is only six weeks after this thing was large enough that I knew it was cancer, and three weeks after the biopsy had almost removed it all. Cancer can be very aggressive.
The plastic surgeon would later enlarge the opening into the shape of an ellipse so that the wound could be sewn shut without puckers. That’s why I ended up with a 2 inch scar. If I could have received treatment at the end of December, when I already knew that it was cancer, then the wound probably would have been no larger than my little fingernail.
Unfortunately, neither surgery went smoothly. During the first surgery, the Mohs surgeon hit an artery, which spurted all over the place. Hey, these things happen and that was no fault of hers. But it wouldn’t stop bleeding, so she had to suture the artery closed. Unfortunately, the nurse handed her sutures which were not dissolvable. Since these would stay below the skin, they had to be dissolvable. So the doctor took out the first set of stitches and put in a second set.
Meanwhile, the local wore off and she had to inject me again. Each round of injections was about 8 shots into my face around the tumor. Since there were two separate rounds of surgery (the first cut hadn’t gone deep enough and the doc had to cut down into the subcutaneous fat in a second round to get it all), and the anesthetic kept wearing off (I’m sensitive to epinephrine, can’t have it, and that is what helps the anesthetic last long enough to keep you numb the whole time) that meant that I had probably 40 injections into my face during the first surgery.
Finally, the first procedure was done. I went to lunch with a big bandage on my face while waiting for my appointment with the plastic surgeon. That’s when things really went bad.
Remember I said that I can’t have epinephrine? Well, the plastic surgeon didn’t remember and he used a local with epinephrine in it despite the fact that we had discussed the issue extensively on my consultation visit. I hadn’t had any epi in about 40 years. My older body reacted to it even more badly than my young one had. I began to feel bad before he had finished injecting my face. My heart started to race and I had trouble breathing. It was like the worst panic attack you can imagine.
I asked him if he had put epi in the anesthetic and he said that he had. I asked him to call the paramedics, because if I had a heart attack as a result, I knew that a plastic surgeon didn’t have the equipment or the knowledge to handle it. I also asked for my son, who was in the waiting room.
The doctor was in full panic mode. He knew he had screwed up, and seemed incapable of acting. The doctor was not taking my vitals, so I asked my son to take my pulse. It was 131 while I was lying down. My son asked the doctor to take my blood pressure. But the doctor didn’t have a blood pressure cuff! He had just moved to the new office and wasn’t unpacked. He didn’t even have any soap by the sink in the room where I was being treated. And he hadn’t had me put on a gown (I had to ask the office assistant for one), and in contrast to the first surgery, I had no surgical cap and no drape either. It was like Third World surgery.
By the time the paramedics arrived, I was pretty much out of it mentally. I had said goodbye to my son, because I thought I was dying.
Fortunately, I didn’t. The paramedics said that my blood pressure was 208/110, if I remember correctly. They did an EKG and found that I was not having a heart attack. They wanted to take me to the emergency room anyway though because BP that high is stroke city. But my body was metabolizing the epinephrine, and my pulse was dropping. My blood pressure fell to 180/100 (more or less, my mind wasn’t working right at the time and I can’t remember) while they were still there.
I had already had so many injections to my face that I wanted this over with, so I declined to go to the ER. And God only knows how long it would have taken to get another appt for wound closure. I couldn’t go around with that big hole in my face. The paramedics strongly recommended that I go as soon as the procedure was finished.
Well, the plastic surgeon was a basket case. My son and I had to calm him down enough so that he was able to finish the procedure. I went to the ER afterward, had another EKG and was released with no treatment despite still having high BP. My BP didn’t drop back to normal until the next day.
My body was so stressed by this experience that I didn’t recover my strength until early March, really just a few days ago. I missed a month of work from being so wrung out physically.
Oh, and that wasn’t all of it. I had the stitches removed a week after the surgery, but the plastic surgeon left one in. I had to go back a week later and have that one removed. He didn’t wear gloves, and I bled with stitch removal. This is not proper standard of care. Now I have to ask myself could this guy be HIV positive or have hepatitis. And it feels like he might have used a non-dissolvable suture at the very end of the wound. So my nightmare still isn’t over. Honestly, I’m getting stressed all over again just thinking about this.
Here are the photos.
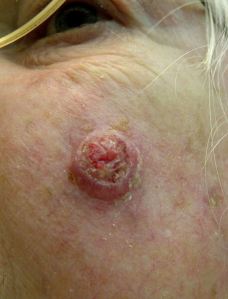
This is my squamous cell carcinoma about three weeks after the biopsy, and on the day of surgical removal. The tumor had looked gone after the biopsy. Note the raised appearance. The cancer went down into the tissue of my cheek as well as outward.

This is the hole that was left in my cheek after the removal of the tumor. Note that I am wearing a surgical cap and a gown. My wound was draped during the surgery, and I was in a surgical suite in the Mohs dermatologist's office. The blackness is due to electrocautery of the open wound. I was a bit swollen and bruised, but no, it didn't hurt. Amazingly I was able to have lunch with no problem.

This is what my cheek looked like after closure of the incision while I'm still on the table. Note how pale I am. I have not manipulated the color. I think I nearly died due to the reaction to the epinephrine. Also note that I am not wearing a surgical cap. The plastic surgeon hadn't even asked that I put on a gown. I had to ask the office assistant for one because I didn't want to bleed onto my clothes. There was no cap, no drape, no surgical light, just a bare office with a table. There wasn't even any soap by the sink! This place was just not set up to do surgery. At least the doctor wore gloves, but he didn't when he removed the stitches two weeks later, and I bled. That is not good.
So that is why I haven’t planted my spring garden yet. I have been utterly exhausted, I suspect from the trauma caused by the epinephrine. I hope to get back to participating in Harvest Monday next week.
Fortunately, squamous cell carcinoma is cured with surgery. No need for chemo or radiation. But it will kill you if you don’t get it removed. If you have a suspicious spot, get it looked at.
Now I just watch and wait to see if the cancer is really all gone. So far, so good. The incision is healing very nicely.



Holy cats! I am so glad you were persistent and knew what was going on. This is clearly a case where you the informed patient saved yourself. Yikes. Heal well and rest up. The garden can wait for you, better to take care of yourself. And thank you for sharing this cautionary tale.
LikeLike
So sorry to hear of your troubles Lou.
I had a similar spot on my back that is now a
large scar. Thanks for sharing your story as
I’m sure it will help someone in the future to be proactive.
LikeLike
WOW, Dr. Lou!!! I was just thinking about you yesterday and wondering why you haven’t posted in so long…. I’m so sorry to hear that you had to endure such a horrible situation compounded by having to wade through such a time- and energy-wasting morass of B.S. to resolve an urgent, life-threatening medical emergency that could have been handled much more efficiently and much less painfully were it not for all the above-mentioned B.S.
May I have your permission to “Facebook” your post? Not only is it helpful in getting the message out re cancer awareness, but it also is an especially striking example of how badly broken the American approach to healthcare is, especially for those who think our system is the best anywhere and oppose any attempt to fix it. Not that “socialized medicine” is perfect, but after living in Japan and France where they had a good delivery system in place for public health services that was simple, accessible, affordable and effective, I hardly ever bother with going to the doctor anymore now that I live here again, even though I have “good” insurance – because it’s such a mind-rending HASSLE!
If it’s of any comfort, my garden “rewarded” me for several months of neglect with an abundance of volunteer mange-tout peas, kabocha pumpkins, tomato plants (no idea which heirloom variety/ies) and an assortment of mystery brassicas all growing beautifully even in the dead of winter. Some of them came from seeds in the home-made compost I finally hastily threw down in late fall after weed-whacking the guava tree and clearing out the remains of summer. I’m sure your gardens will be at least as understanding 🙂
LikeLike
I am so sorry you had to go through all that. There are two excellent lessons in your story. The first, to be proactive about your health care. The second, to take control. I often wonder if with my own round of cancer in 2009, if I hadn’t fired the first hospital (that missed the tumor twice, even when I pointed it out to them beforehand), if I’d even still be here. After transferring hospitals, the administrative system was so bogged down, it took two MONTHS for surgery to remove the tumor…which ran amok in the meantime. I find it infuriating that these days patients almost have to bully doctors into doing their job well. I’d run a mile from that plastic surgeon, and also be tempted to report his incompetence to the medical board.
In the meantime, I’m very glad to hear that despite it all, you’re now feeling improved, just in time to enjoy some beautiful spring weather. Your garden will still grow, just perhaps not quite as intended for the early part of the season, but hopefully things will be back to normal very soon, and this will all be a distant memory.
LikeLike
Oh my! What a horrible experience! Rest up, allow for healing, and know you are in my thoughts.
LikeLike
Bee Girl, Brenda, Shelley, Clare and Ali, thank you so much for your comments. Yes, Brenda, you may post a link to my website on your Facebook page. Our health care system is truly a mess. Now my HMO is denying coverage for the ER visit that the paramedics told me to make. So the agony goes on. Meanwhile, the scar is healing nicely. The physical one, that is. The emotional one continues.
LikeLike
What a story! If it makes you feel any better, I had MOHS surgery last Wed for a basal cell carcinoma which was there for months and months and was maybe 3.5 mm. I have a 1.25 inch scar. Stitches removed today. Puffy etc. And this MD was highly regarded. Johns Hopkins etc.
LikeLike
RobK, I hope it heals quickly. My scar is now invisible and it has been only four months since surgery. All’s well that ends well.
LikeLike
This is really scary as I have a keratoacanthoma and its pretty big on my nose and its sche to be removed on wed. Ive had it for about 6 weeks now.
LikeLike
Connie, I hope all went well for you.
LikeLike
WOW..I hear ya loud & clear.. I have had sooo many KA/SCC on my body for over 15 yrs now. Many were excised surgically..and other had Moh’s surgery..and many have had injections of steroids..intralesional injections. Mine have all been VERY painful lesions !! That usually works..IF dont when lesions are not too big..takes months to go away..& for the big scabs to fall off..Not pretty. Just wanted to thank U for posting this..Not many people understand exactly what KA’s even are..I have never met another person with them..thought It was only me..thanks again.. Also ..I don’t want to burst your bubble.. but always be on the look out for any other ones..My come non stop..!!
LikeLike
Susan, I am well aware that Actinic Keratoses come back. Again and again. And sometimes they develop into cancer again. Be vigilant. BTW, AKs are very common, esp in people with fair skin.
LikeLike
I am currently going through the similar process. On March 27, I went to my family doctor and after looking at my leg she stated it was Squamous Cell Cancer and sent me to a dermatologist. A week later was at the dermatologist where I was told the same, that is was Squamous cell cancer, measuring in at 17 X 17. It is on the back of my leg. THat Monday it was biopsied and on Friday was confirmed it was cancer and that I would need a plastic surgeon for a skin graft. Saw the plastic surgeon on 4/15, to let him see it. Had the actual procedure on 4/22. I have stayed off of it but at 5 days it started bleeding. Drs office told me to change the bandage which I did. The next day brown liquid was coming from it. It appears to be the ointment and blood. So, I cleaned it up again, wore a pressure bandage for a couple of hours. That was a couple of hours ago. I am 46 years old. I am fair skinned with blue eyes. I am hoping and praying I am on the road to recovery.
04/28/13
LikeLike
I am your typical strawberry blonde age 60 plus with a history of SCC and BCC along with the usual actinics…..this time I got in one day after the call with an excellent derm…bummer…did not get it all per the biopsy and going back in 2 weeks for 10mm (5mm already gone). He is recommending a Blue Light chemo photo treatment for my arms, hands, face and chest (this SCC is on my chest..prior in my eyelid and nose) have any of you done the Blule light special? 3 sessions is what he isrecommending…yes I too am a scar body……………………..
LikeLike
Thank ypu so much for posting your story. I’ve had a small lesion on one eyelid for months that wouldnt go away. Finally got it biopsied and found it to be SCC, surprising both my eye doc and the eye surgeon. Its been 3 weeks since the biopsy and my insurance says the reconstruction will take 30 more days to approve. The plastic surgeon’s staff tells me they will not schedule surgery, even if I pay for it, until approval is received and I should relax and be “patient”, despite the doc insisting this be removed within a month. I see another plastic surgeon this week for another opinion because I’m through being patient.
LikeLike
Sandy, I haven’t been checking my blog all that often. Hope you got your issue resolved, and best wishes.
LikeLike
That was very informative, I hope you are feeling better and this stuff is just a memory now.
LikeLike
Yep, a very bad memory, plus a long faint scar on my face. Thanks Sara.
LikeLike
SCC’s and BCC’s are easy to remove with Black Salve. I know because I have used it for years …it is inexpensive, leaves virtually no scar – given time, It certainly can look a bit scary if used on a big lesion, but does a far neater job than the knife or other dreaded remedies such as Radiation.
LikeLike
Ken, I would not risk doing anything other than medically approved procedures with either Basal Cell Carcinoma or Squamouos Cell Carcinoma. Either type can kill you if not removed. I have no idea what Black Salve is, but surgery is the quick and sure-fire way to remove them, no chemo or radiation needed. Basal Cell Carcinomas can usually be treated with liquid nitrogen for fast results.
LikeLike
This is an interesting and informative post, thanks for making it. I would like permission to post a link to it on my Facebook page (https://www.facebook.com/cdozo) if that’s OK with you.
LikeLike
No, Ca Dozo I would rather you didn’t.
LikeLike
Thanks for your story. It will prove to be very helpful . I have an HMO for the first time this month after my cobra insurance expired. I went to my own dermatologist and was diagnosed with keratoacanthoma . Now waiting for them to approve my referral for plastic surgeon, after attending the clinic To which I was assigned . I will be very pushy if not approved tomorrow. Have appointments set up ,but no referral yet. I can see it grow daily and have my sons wedding to attend in less than a month. Wish me luck !!!!!!
LikeLike
Rosemary, I have not been very good about keeping up with my blog. How did your surgery go? It takes a while for those surgery scars to go away. Yours should be looking good by now.
LikeLike
Thank you so much. I hope and trust you are doing well. You have helped me. I thought I had a skin tag on my upper chest. But in three weeks, it kept growing and I made an appointment with my dermatologist. She removed it (it was about 1/4 inch in diameter.) She cut it off and then burned the site. I am going back tomorrow for the follow up. My questions are , did she get all of it? How does she know? If not, what do we do next.? I am trying not to over react. But I am worried. Thank you again.
LikeLike
Amy, a simple freeze is a good first step. Squamous cell carcinomas rarely metastasize. If the freeze did not get all of the “deep roots” of the cancer, it will come back. Then the option is Mohs surgery like I had. My cancer has not come back.
LikeLike
Dear Sir, I had a biopsy 2 weeks ago and it is an aggressive SCC. It is on my forehead and looks just like yours did after 3 weeks. I felt something was going wrong so I am reassured after seeing and reading your post. My Mohs surgery is in 2 weeks so i guess it is not unduely delayed. And thanks to your generousity I now know what to expect. Posts like this are so valuable for others experiencing the unknown.
LikeLike
Sorry it has taken me so long to get back to you. I hope your surgery went well.
LikeLike
I ha a one inch scaly spot on arm it was cationic keritosis. It came back ten years later just pink and dry. Anyway I got a bad feeling from this Dr first visit. He seemed hyper and bragged about how many mohs he’s done. My spots
were treated as one coz so close together. I ended up 30 stiches and flap surgery. He is without a doubt knife happy. I’ve cancelled my other appointments
LikeLike
The term is “actinic keratosis.” They can develop into cancers. Hope you are OK now.
LikeLike
Yikes, Colleen. A one-inch spot is a big one. BTW, the term is actinic keratosis. Those are pre-cancerous. Auto correct may have changed it to cationic, which is a word. How did your procedure work out?
LikeLike
I was just confirmed to have squamous cell carcinoma on my back. It is probably the size of a 50 cent piece. They said it is a normal type of skin cancer and they have to go in deeper and wider to cut mine out. With the size of mine I am a little worried on how far deep and wide they actually have to go. When I first had it my family dr told me that it was fine nothing to worry about, however I turned around and broke my ankle in 3 places and had to be on bed rest for over 5 months on my back with my leg raised. Needles to say during that time it broke open and began to grow, then it practically went away almost then reformed but a lil bigger. This has been going on for over a yr so I decided to go have it looked at by dermatologist. That is when they cut it off and just got my results yesterday. They said I will be ok and they want me to go back in January to have it removed so I am curious how long is too long? I just want it out of me.
LikeLike
Crystal, best of luck to you. The good news about squamous cell carcinomas is that they very rarely metastasize (spread). But it can kill you if ignored, because it can invades other tissues. When the doc goes to remove it, he/she should use Mohs technique, where they examine (using a microscope) each piece removed to make sure that they got it all. Good for you in bypassing your family doctor to get a second opinion from a dermatologist. That probably saved your life. Expect the wound to weep for a couple of weeks. You will probably have to change the bandage fairly often in the beginning. But all should be fine in the long run. Best wishes. Stop by again and let us know how it went.
LikeLike
Hi there im familiar as well w this. I had my first Keraochantoma a little over 3 years ago. I had extensive surgeries and plastic surgeries. Unfortunately after all this time developing another one on the same exact spot on my nose but opposite side.Its been on there not quite 2 weeks. I happen to have a appt w my PCP on Mon. Im hoping to get a referral to a dermatologist. Ive also setup a app out of network in case w a dermatologist. My hope is that i can shave as much time as possible and hopefully they can just freeze this thing without going through the Mohs and the extensive plastic surgery i needed to fix my nose. I cant believe it just went i thought i wouldnt get another one it pops up. It sucks because after all this time i started to date again and now this.
LikeLike
Hi i had my first Kerachantoma at 39. It took extensive surgeries and extensive plastic surgeries to fix my defect. Unfortunately a little over 3 years and another has popped up. Exact spot but on opposite side of nostril. Its been about 2 weeks and i was hoping it wasnt what i thought it was. I happen to have a appt w my PCP in two days. Im hoping to get a referral and to try and get this taking care of ASAP. The first time i had no idea what it was and had let it go 2 mos before i started to seek med attention. Of course by the time i had got to the point where it was to be removed another 2 mos had passed by. Im hoping if i can shave off as much time as possible they can freeze it and not have to go through the surgeries i had to go the first time around.
LikeLike
I hope you got your issue taken care of satisfactorily and in a timely manner.
LikeLike
Thanks i had a biopsy they are saying its just a wart this time. I go tomorrow for a followup.
LikeLike
OMG what a horrendous experience you have had. I have a lump on my quad which looks like your initial photo.I gave had it a few months and only got it checked 2 weeks ago. I received an appointment this morning for Thursday this week with dermatology. At the time the G.P indicated that she thought it was nothing to worry about, but will know more after the dermatology appointment. I Have been using eggplant cream as a poltus which seems to have reduced it a bit, so fingers crossed. I Hope you are recovering well 💛
LikeLike